The Centers for Advanced Orthopaedics is redefining the way musculoskeletal care is delivered across the region with locations throughout Maryland, DC, Virginia and Pennsylvania.
Tips for Identifying & Treating Flatfoot
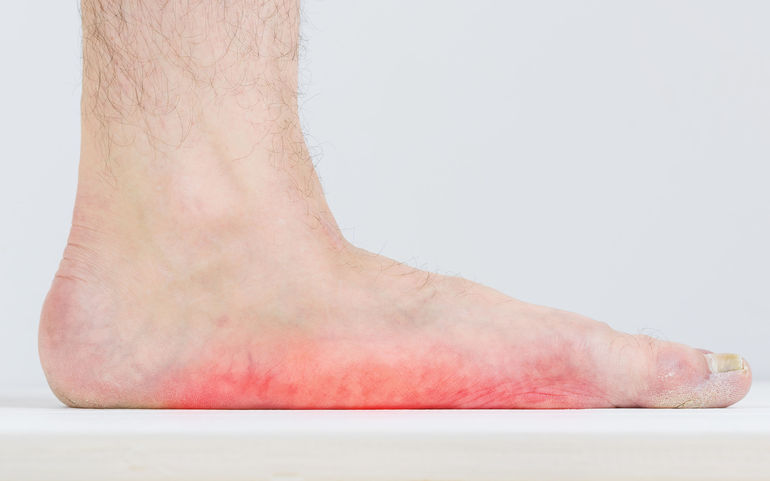
Tendons connect muscles to bones and stretch across joints, enabling you to bend that joint. One of the most important tendons in the lower leg is the posterior tibial tendon. This tendon starts in the calf, stretches down behind the inside of the ankle and attaches to bones in the middle of the foot.
The posterior tibial tendon helps hold your arch up and provides support as you step off on your toes when walking. If this tendon becomes inflamed, over-stretched or torn, you may experience pain on the inner ankle and gradually lose the inner arch on the bottom of your foot, leading to flatfoot.
Flatfoot Signs & Symptoms
- Pain and swelling on the inside of the ankle
- Loss of the arch and the development of a flatfoot
- Weakness and an inability to stand on the toes
- Tenderness over the inside of the ankle when active
Risk Factors
- Women over 50 years of age
- Obesity
- Diabetes
- Hypertension
- Previous surgery or trauma (ankle fracture)
- Inflammatory diseases such as Rheumatoid Arthritis
Diagnosis
The diagnosis is based on both a history and a physical examination. Your physician may ask you to stand on your bare feet facing away from him/her to view how your foot functions. As the condition progresses, the front of the affected foot will start to slide to the outside. From behind, it will look as though you have "too many toes" showing. You may also be asked to stand on your toes or to do a single heel rise: stand with your hands on the wall, lift the unaffected foot off the ground, and raise up on the toes of the other foot. Normally, the heel will rotate inward; the absence of this sign indicates posterior tibial tendon dysfunction. Your doctor may request X-rays or a magnetic resonance image (MRI) of the foot.
Treatment Options for Flatfoot
Without treatment, the flatfoot that develops from posterior tibial tendon dysfunction eventually becomes rigid. Arthritis develops in the hindfoot. Pain increases and spreads to the outer side of the ankle. The way you walk may be affected and wearing shoes may be difficult.
The treatment your doctor recommends will depend on how far the condition has progressed. In the early stages, posterior tibial tendon dysfunction can be treated with rest, non-steroidal anti-inflammatory drugs such as aspirin or ibuprofen, and immobilization of the foot for 6 to 8 weeks with a rigid below-knee cast or boot to prevent overuse. After the cast is removed, shoe inserts such as a heel wedge or arch support may be helpful. If the condition is advanced, your doctor may recommend that you use a custom-made ankle-foot orthosis or support.
If conservative treatments don't work, your doctor may recommend surgery. Several procedures can be used to treat posterior tibial tendon dysfunction; often more than one procedure is performed at the same time. Your doctor will recommend a specific course of treatment based on your individual case.